
Paul Spicker
Health care
Health
There are many definitions of 'health'. They include:
- cultural definitions: health is a standard of physical and
mental well being appropriate to a particular society.
- normative definitions: health as an fixed level, or an ideal
physical and mental state
- functional definitions: health is a state of being necessary to
perform certain physical and mental activities
Health depends on a number of factors, including biological
factors, environmental factors, nutrition, and the standard of living.
In other words, health can be seen as a function of welfare. Few of the
issues which cause ill health are dealt with directly by 'health
services'; they are, rather, issues in the 'welfare state' as a whole.
When, in the 19th century, Chadwick identified poor health as a major
cause of pauperism, his response was to improve sanitation, not to
introduce more extensive medical care. Most of the world's diseases are
attributable to poor water supply or nutrition. 'Health services' are
better described as medical services.
External links: Our world in data - global health
Inequalities in health
There are clear differences in the incidence of ill health by
social class. Figures from the UK show that people in lower social
classes, including children, are more likely to suffer from infective
and parasitic diseases, pneumonia, poisonings or violence. Adults in
lower social classes are more likely, in addition, to suffer from
cancer, heart disease and respiratory disease.
There are several possible explanations for these inequalities.
- artefact explanations. Both 'health' and 'social class' are
artificial categories constructed to reflect social organisation.
- natural and social selection. This would depend on the view that
people who are fittest are most likely to succeed in society, and
classes reflect this degree of selection.
- poverty leads to ill health, through nutrition, housing and
environment.
- cultural and behavioural explanations. There are differences in
the diet and fitness of different social classes, and in certain habits
like smoking.
There are often major inequalities in access to health care
according to social class. The problem becomes what Tudor Hart once
called an 'inverse care law'; that those people in the worst health
receive the least services. [2]
Health care
Health care can be divided into a number of different branches.
Conventionally these include
- hospital care. Hospitals can be distinguished between
acute and long-stay care. Acute care covers the full range of medical
specialties: long stay care has principally been used for psychiatric
care and continuing nursing care. The current trend is for long stay to
be minimised and for acute hospitals to offer a full range of care.
- primary care. Primary care refers to basic medical
treatment and non-hospital care, including general or family
practitioners, professions ancillary to medicine (including dentistry,
optics and pharmacy) and domiciliary health care (home nursing,
occupational therapy, etc.). In some countries, the preferred
distinction falls between hospital and "ambulatory" care. Ambulatory
care includes primary care and most day care in hospital.
- public health. This field includes not only
preventive medicine (e.g. screening, inoculation or health education)
but also several areas not necessarily linked with conventional health
services, including housing, water supplies, sewerage and food hygiene.
Public health is probably the most important issue for the health of
a population; primary care is the main focus of medical care in
practice. Medicine in hospitals is probably the least important in
terms of its impact on health or illness, but it costs the most, has
the highest status and is the focus of most political attention.
That does not mean, however, that medical systems miss the point - they
are the point. What people mainly look for in a health system is
not health, but social protection in the event of illness; and a
national health care system offers, not health, but universal
coverage.
External link: Priorities
in health care: international comparisons |
The Commonwealth Fund compares health care systems in
different countries
Financing health care
Debates about "health services" are not just about health care. The
term stands for a range of measures concerned with social protection.
These measures typically include social insurance and solidaristic
provision. In some countries (e.g. France) this is classified as a form
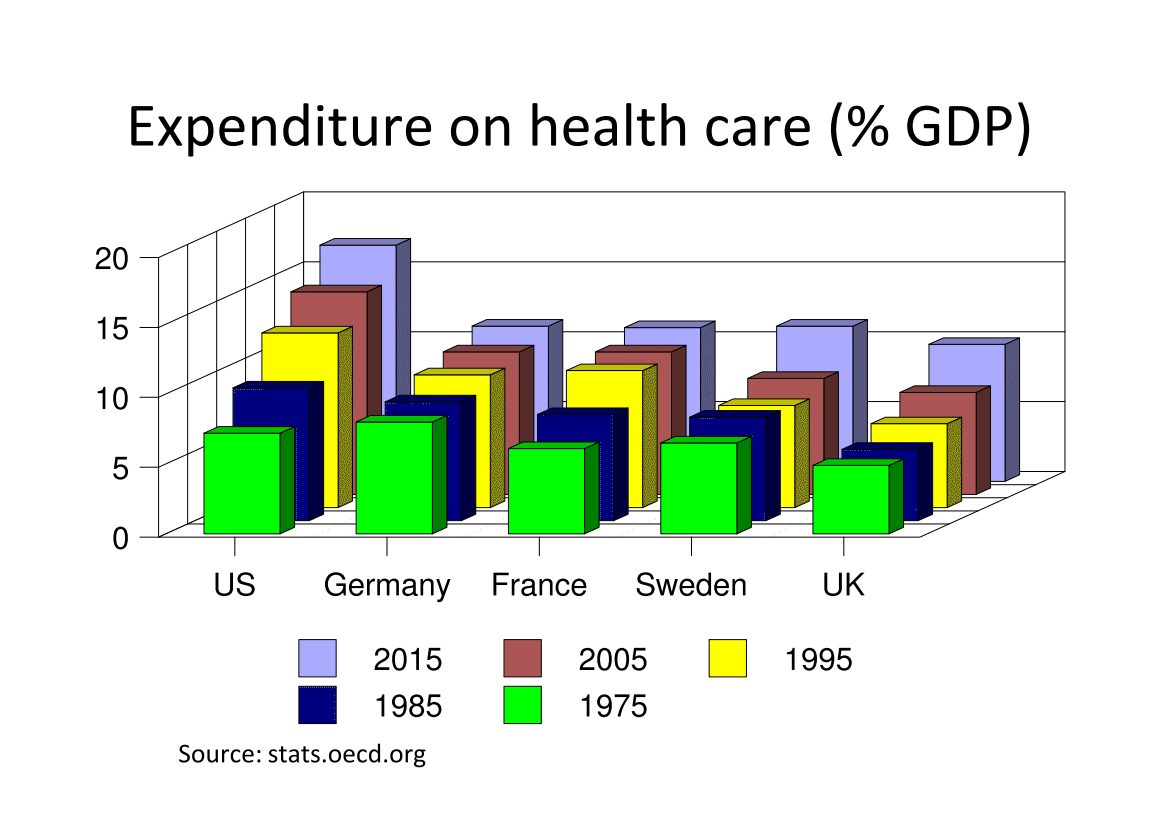
of social security. Most countries in the OECD, with the main exception
of the USA, offer universal coverage for the costs of medical treatment
in hospital, and for at least part of the costs of ambulatory care.
Payment for medical goods, such as pharmaceuticals, is much more uneven.
 When people pay for social protection,
their
expectations are likely to be different from consumers paying for
specific courses of treatment, like elective surgery. Typical issues in
social protection are accessibility, coverage and the responsiveness of
services, especially in emergency. These issues are different, and
potentially more important for service users, than the kinds of issue
which influence decisions in direct consumption, such as quality or the
availability of alternative treatments. However, many debates in health
care, such as arguments for "centres of excellence" in medical care or
arguments for developing choice, ignore the former criteria in favour
of the latter.
When people pay for social protection,
their
expectations are likely to be different from consumers paying for
specific courses of treatment, like elective surgery. Typical issues in
social protection are accessibility, coverage and the responsiveness of
services, especially in emergency. These issues are different, and
potentially more important for service users, than the kinds of issue
which influence decisions in direct consumption, such as quality or the
availability of alternative treatments. However, many debates in health
care, such as arguments for "centres of excellence" in medical care or
arguments for developing choice, ignore the former criteria in favour
of the latter.
The focus on insurance and security implies a strong focus on
financial issues. The combination of ageing populations, increasing
expectations and demand, rising technical costs (or "medical
inflation") and increasing costs of labour in developed economies have
led to substantial increases in expenditure. State-provided care tends
to be relatively cheaper than market-based provision, partly because of
rationing, partly because consumer demand is less restrained, and
partly because producers are less free to determine expenditure.
Health care in Britain
The development of health care in
Britain
Medical care in the nineteenth century was principally private or
voluntary. However, sickness was a primary cause of pauperism, and the
Poor Law authorities began to develop their own infirmaries for sick people. The demand for the infirmaries was at first resisted by a deliberate
emphasis on the stigma of pauperism, of which the main legal
consequence was the loss of the vote. Few people who became paupers had
the vote, but after the extension of the franchise in 1867 and 1884,
the numbers increased dramatically. In 1885, the law requiring people
to be paupers before using the infirmaries was abolished. Public
hospital building increased after the foundation of the
Local Government Board in 1871, reflecting the influence of doctors in
the central administration; there were surges in numbers built in the
1870s and 1920s.
Prior to 1948, health services were mainly based on three sources:
- Charity and the voluntary sector.
- Private health care. Hospitals were fee paying or voluntary;
primary care was mainly fee-paying or insurance-based.
- The Poor Law and local government. Poor Law hospitals were
transferred to local government by the 1930 Poor Law Act.
These were unified when the NHS was formed in 1948.
External link: NHS history
The NHS in
principle
The right to welfare. The NHS is seen by many people as the
core of the 'welfare state'. People receive health care as a right.
This is not a right to health care on demand. The principal rights are
a
right to be registered with a general practitioner, and the right to be
medically examined, though out of practice hours that examination has
been
substantially delegated to NHS 24, a telephone-based service. There is
no formal right to receive any specific treatment. This is within the
discretion, or 'clinical judgment', of the doctor.
Comprehensiveness. The NHS is held to protect all citizens.
Access to health services depends on registration with a general
practitioner. Homeless people in particular have great difficulty
gaining access to primary care, because without an address it is
generally impossible to register.
The service itself has never been comprehensive. The NHS does ration
resources according to priorities. Not only are there not regular
checkups for everyone, but there are long waiting lists, and people
with quite serious needs - like those from the 1950s onwards needing
renal dialysis - may die, because the cost of treatment is greater than
the NHS is ready to bear. NICE, the National Institute for Health and
Clinical Excellence, approves medicines for use on the basis of the
cost per Quality Adjusted Life Year or QALY; approval seems to depend
on cost not exceeding £20-30,000 per QALY, though the level is higher
for end-of-life care.
A free service at the point of delivery. The initial idea
was that no-one should be deterred from seeking health services by a
lack of resources. Charges were first introduced by the Labour
government in 1950. They were substantially increased by the
Conservative government after 1979. The 1988 Act removed free eye
tests, later restored in Scotland.
Social protection.
The NHS offers all citizens - whether or not they actually use the
service - the equivalent of medical insurance. This has a
clear and direct financial value, but that value is rarely
recognised, and it does not feature in national income or distributive
assessments.
External links: A debate: universal
health care or rationing?
The NHS and the hospitals
Throughout its history, the NHS has been dominated by the hospital
services, in particular by the high-status university hospitals. The
bulk of expenditure on the NHS (over 70%) goes on hospitals. General
practice, though it deals with the vast majority of reported illness -
probably over 95% - accounts for less than 10% of spending.
The NHS inherited a maldistribution of resources, especially in
London, where the main acute hospitals were concentrated in the centre of the
city. London's lack of adequate primary care coverage and over-reliance
on hospitals for treatment have created recurring problems ever since.
The Labour
government in the 1970s attempted to redress the balance by
transferring resources from hospital care to primary care, limiting the
growth of better served regions, and favouring the development of some
underfunded specialties, like medicine for the elderly. This led to
hospital closures, in a policy often identified at the time with 'community care'. The policy was continued by the Conservatives in the
1980s.
Complaints about the NHS tend to focus on the problems of acute
hospitals:
waiting lists, lack of spare capacity, and 'shroud-waving' in response
to spending controls. The severity of the problems is possibly
exaggerated. Enoch Powell, a former Minister for Health, commented on
"the continual, deafening chorus of complaint" which characterises the
NHS. By contrast with the private sector, where people always pretend
that things are better than they are, the system of finance in the NHS
"endows everyone providing as well as using it with a vested interest
in denigrating it. " [3]
Opinion: Reforming A&E in Scotland
The organisation
of the NHS
 It
is sometimes suggested in the
press that the NHS has not really been
reformed since its foundation; the opposite is true. Initially, the NHS
had a tripartite (three-part) structure, with
three branches - hospitals, primary care and local authority health
services. In 1974, a 'unified' administrative structure was introduced,
with three
main levels of management, at Regional, Area and District level. The
1974 reorganisation led to a great deal of disruption, and was heavily
criticised. Following political disagreements, Area Health Authorities
were abolished in 1982 - discarding ideas like local
integration of services and co-ordination with social services
authorities.
It
is sometimes suggested in the
press that the NHS has not really been
reformed since its foundation; the opposite is true. Initially, the NHS
had a tripartite (three-part) structure, with
three branches - hospitals, primary care and local authority health
services. In 1974, a 'unified' administrative structure was introduced,
with three
main levels of management, at Regional, Area and District level. The
1974 reorganisation led to a great deal of disruption, and was heavily
criticised. Following political disagreements, Area Health Authorities
were abolished in 1982 - discarding ideas like local
integration of services and co-ordination with social services
authorities.
In the 1990s, the role of Regional
Health Authorities was taken over by 8 regional offices of the NHS
management executive. For the first time, Klein comments, the NHS
became truly a nationally administered, centralised service. [4]
The reform of
services in 2002 replaced the English Regional Health Authorities and
District Health Authorities with 28 new Strategic Health Authorities
and 310 Primary Care Trusts; the number of SHAs was reduced to 10 in
2006. These authorities were abolished in the 2012 Health and Social
Care Act, which now relies on the role of a large number of "Clinical
Commissioning Groups" in their place. In England, central control
has passed
from the Department of Health to NHS England and Monitor, the health
care regulator. In Wales and Scotland, this authority has passed to the
devolved administrations.
External links: National Health Service
The NHS and quasi-markets
In the 1980s, Enthoven, an American economist, made an influential
criticism of the NHS, arguing that it was inefficient, riddled with
perverse incentives and resistance to change. [5] Enthoven
argued for a split between purchaser and provider, so that Health
Authorities could exercise more effective control over costs and
production.
The development of an 'internal market' in the 1990s was based in
the belief that the NHS would be more efficient
if it was organised on something more like market principles - not a
real 'market', but a quasi-market.[6] The NHS administration was
broken up into quasi-autonomous
trusts from which authorities bought services. In principle, the Labour
government removed the internal market. In
practice, it retained its main elements - the purchasing role of health
authorities, the provider trusts and GP commissioning. In England,
routine service
provision is now governed through commissioning and detailed contracts;
most contracts since 2012 have been awarded to private providers.
The
emphasis on
commercialisation and sub-contracting has been heavily
criticised.
Part of the objection has been to the introduction of the profit motive
in health care. More fundamentally, the private sector works to
different criteria from the public services. "Choice" in the market is
not
only choice for a patient; it also implies choice for the
provider. Market provision and competition depend on producers
selecting the tasks to be done and the populations to be served, and
that may be inconsistent with the broader
objectives of
the NHS.
While there are continuing concerns about the effects of
marketisation, there are also many criticisms of 'command and
control' from the centre. The Francis
report on the Mid-Staffordshire hospitals points to an
inappropriate focus on government-led financial control and targets at
the expense of patient care. It is not clear whether both
types of
criticism - centralised control and market-based fragmentation - can be
valid
at the same time.
External links: Allyson Pollock on the 2012 reforms (video)
References
- P Townsend, N Davidson, M Whitehead, 1990, Inequalities in
health, Penguin.
- J Tudor Hart, 1971, The inverse care law, Lancet 1 405-12.
- J E Powell, 1966, A new look at medicine and politics, Pitman.
- R Klein, 1995, The new politics of the NHS, Longman.
- A Enthoven, 1985, Reflections on the management of the NHS,
Nuffield Provincial Hospitals Trust.
- J Le Grand, W Bartlett, 1993, Quasi markets and social policy,
Macmillan 1993.
Further reading
J Naidoo, J Wills, 2008, Health studies: an introduction
Basingstoke: Palgrave Macmillan
A Mahon, K Walshe, N Chambers, 2009, A reader in health policy and
management, Maidenhead: Open University Press
Health services, from the British Library's
Social Welfare Portal
 When people pay for social protection,
their
expectations are likely to be different from consumers paying for
specific courses of treatment, like elective surgery. Typical issues in
social protection are accessibility, coverage and the responsiveness of
services, especially in emergency. These issues are different, and
potentially more important for service users, than the kinds of issue
which influence decisions in direct consumption, such as quality or the
availability of alternative treatments. However, many debates in health
care, such as arguments for "centres of excellence" in medical care or
arguments for developing choice, ignore the former criteria in favour
of the latter.
When people pay for social protection,
their
expectations are likely to be different from consumers paying for
specific courses of treatment, like elective surgery. Typical issues in
social protection are accessibility, coverage and the responsiveness of
services, especially in emergency. These issues are different, and
potentially more important for service users, than the kinds of issue
which influence decisions in direct consumption, such as quality or the
availability of alternative treatments. However, many debates in health
care, such as arguments for "centres of excellence" in medical care or
arguments for developing choice, ignore the former criteria in favour
of the latter.



 It
is sometimes suggested in the
press that the NHS has not really been
reformed since its foundation; the opposite is true. Initially, the NHS
had a tripartite (three-part) structure, with
three branches - hospitals, primary care and local authority health
services. In 1974, a 'unified' administrative structure was introduced,
with three
main levels of management, at Regional, Area and District level. The
1974 reorganisation led to a great deal of disruption, and was heavily
criticised. Following political disagreements, Area Health Authorities
were abolished in 1982 - discarding ideas like local
integration of services and co-ordination with social services
authorities.
It
is sometimes suggested in the
press that the NHS has not really been
reformed since its foundation; the opposite is true. Initially, the NHS
had a tripartite (three-part) structure, with
three branches - hospitals, primary care and local authority health
services. In 1974, a 'unified' administrative structure was introduced,
with three
main levels of management, at Regional, Area and District level. The
1974 reorganisation led to a great deal of disruption, and was heavily
criticised. Following political disagreements, Area Health Authorities
were abolished in 1982 - discarding ideas like local
integration of services and co-ordination with social services
authorities.